The 8th Annual eMental Health International Congress was held at the Pullman Hotel in Auckland over two days on November 10th and 11th, 2022. The event was live streamed to 15 countries, with over 40 speakers focussing on the theme: Mental Health’s Transformation – Bringing The Digital Ecosystem To Life.
Due to consistent sell-outs in the past, this year for the first time the Congress was open to the public worldwide with large participation from international research groups, Governments, healthcare organisations, people with lived experience and product developers.
Of special note were key Government representatives from the United States, Canada, Australia, New Zealand, the UK, Sweden, Singapore, and the Philippines. They were all in attendance to explore strategies for implementing eMental Health at national level and learn from one another. This unprecedented commitment to cross-border collaboration at the Congress was a landmark in the evolution of global mental health.
Thursday 10th November
Welcome and Framing Remarks
The Congress was officially opened by kaumātua, George Hill [Ngāti Whātua] who welcomed international delegates to Aotearoa, New Zealand and invited participants to reflect on the purpose of their work with a Māori proverb:
He aha te mea nui o te ao
What is the most important thing in the world?
He tangata, he tangata, he tangata
It is the people, it is the people, it is the people
Our vibrant and energetic MC Taimi Allan then took the stage to welcome everyone to the Congress, giving special mention to participants with lived and living experience of mental illness.
Opening remarks were then delivered by Christine Morgan, eMHIC Board Chair and CEO of the National Mental Health Commission of Australia, Minister for Health in New Zealand Hon. Andrew Little and Anil Thapliyal, Executive Director of eMHIC.
Christine reaffirmed the importance of participation by those with lived and living experience and the cruciality of cross-border collaboration as we work together to implement eMental Health best practice around the world.
Health Minister Andrew Little, spoke about how as the digital world grows and becomes an even more integral part of our lifestyles, so too should our capability to provide eMental Health support when, where and in ways that work for people.
Anil shared his thoughts on the current state and future of eMental Health. Scalable activation, he said, is not just about creating standards, it’s about getting the entire ecosystem right.
Keynote: Pat Deegan, Founder of Pat Deegan PhD & Associates
The presentations were opened by the inspirational Pat Deegan. Pat is a disability-rights advocate and thought-leader in the field of mental health recovery, bringing a message of hope for recovery to audiences around the world. Pat’s keynote address was titled ‘Start, Sustain, Spread’ which explored the key steps Pat has taken to create and grow the Common Ground peer support service. Coming from lived experience of schizophrenia herself, Pat’s company was founded by and for people in recovery.
Common Ground capitalises on the amount of time people spend in waiting rooms before their medical appointments to deliver a digitally enabled peer support service. The programme has transformed a previously inert half an hour into an active and empowering pocket of time used to prepare the individual for their upcoming psychiatric appointment through a peer run decision support centre.
Common Ground has had over 100,000 logins over the past 5 years with 25,000 users, evidencing the successful implementation of the service.

Pat Deegan (right) visiting a Common Ground peer-run Decision Support Center.
‘Let’s Collaborate’ Group Activity
Gregor Henderson, eMHIC Board Member and former Director of Public Health England facilitated an interactive session designed to create a collaborative environment within the Congress.
International leaders presented on topics they had discussed during a pre-Congress “Think Tank”. The presentation topics were: Prejudice and Discrimination, Promotion and Prevention, Workforce Development, Healthcare Industry, and Evidence Creation.
Afterwards, Gregor facilitated a group activity whereby Congress participants (both in the room and online) were prompted to identify three major problems facing their mental health system, and brainstorm digitally-enabled solutions and government actions for each of them. Groups captured the outcome of their discussions on a single-page worksheet.
The valuable insights from this activity will be used by eMHIC to help inform government mental health strategy discussions in eMHIC’s member countries around the world.
Keynote: Dr Julie Smith, Clinical Psychologist, Online Educator and Bestselling Author
Julie opened her presentation with a question; “How many people in your life do you feel close enough to, to share a personal problem with?” In a national survey in the US, the mean number was 2 and the mode was 0 – ¼ Americans feel they have no one they can go to with their personal problems .
Through her own practice, Julie found that many of her clients found the educational aspect of therapy empowering, and she started to wonder why this information wasn’t more easily accessible. This led her to write her #1 UK best-selling book “Why Has Nobody Told Me This Before?” and begin delivering successful content to millions of users on social media, which was where she realised everyone’s attention was.
Julie describes getting creative with delivering scientific information – you can’t simply put out a journal article, but need to translate it into fun and engaging content that the public can not only understand, but enjoy viewing. Julie showcased some of her most popular videos that have amassed millions of views across the various popular social media apps i.e. TikTok, Instagram, Youtube.
She closed her talk by discussing how as a scientific and technological industry we focus on tech and looking at what technology enables us to do. However what is truly important, she described, is connecting with your audience; making people feel seen, heard and valued by a human being.
She ended with a powerful statement and call to action: “Technology is only truly useful if it focuses on real human need, so always always start with the person, not the tech.”
Brag & Steal: Pioneering Change
A brag and steal session is an opportunity for individuals and organizations to brag about their success stories and Congress attendees to steal ideas to implement in their own work.
Chris Wright is the National Advisor for Digital Mental Health in Scotland, which was a role created in 2020. Chris’ role is shared across two parts of the Scottish Government; the Digital Health & Care Directorate, and the Mental Health Directorate. Chris described the introduction of his role as key because it required him to connect two different directorates together, something which had rarely happened.
Scotland is embedding digital at the heart of Government mental health programmes. Chris described in detail the various ways that digital mental health is being embedded and integrated into Scottish Government services and systems. This includes implementing a stepped care model, and using it across a huge variety of mental health services ranging from youth to perinatal to within prisons.
Achieving clinical and public acceptance of digital is a core goal, and Scotland achieves this through influencing clinical guidance at a national level, developing clinical leadership, and fostering digital inclusion and equality.
Nicholas Watters is the Director of Access to Quality Mental Health Services at the Mental Health Commission of Canada (MHCC). Nicholas’ talk focused on the recent App Accreditation Framework that the MHCC has developed with ORCHA.
Nicholas demonstrated the need for the framework through some simple statistics such as that there are currently 21,000 mental health apps available, but many apps are not created on sound evidence. He quoted a study from the Lancet in 2019 which looked at the top 700 mindfulness apps that you could download; of these, only 23 were delivering true mindfulness training, and only 1 was based on empirical evidence.
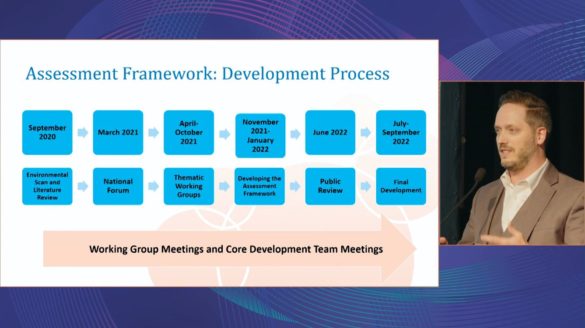
Nicholas explained that Canada knew they were not alone; they are not the only country in the world facing this challenge. They didn’t want to reinvent the wheel, which is done all too often in healthcare. So, they did an environmental scan and literature review of what already existed and partnered with ORCHA to form a Canadian-specific app assessment framework.
A large-scale co-design process was used, which included people with lived and living experience, policy makers, clinicians and app makers. Common themes that emerged across all of the groups were cultural safety, social responsibility and equity, and so a specific working group was developed that focused specifically on these themes.
Once developed, the final step was to take the framework to the public for review. The public was asked what they thought of the framework and if it would be useful. Their response was overwhelmingly positive.
Nicholas explained that the next step is to get the framework off the shelf via a digital formulary. This will mean any person living in Canada can go on the site and get access to validated and safe apps, either for personal use or, in the case of practitioners, prescribing safe and effective apps to patients.
Fiona Costello, Vice President of National Accreditations at ORCHA discussed the need for assessment of mental health apps in regards to safety and effectiveness. With only 18% of the 4,000 mental health apps meeting quality thresholds, how do we know which apps are safe and effective for use?
ORCHA is helping the workforce and the consumer to build confidence in mental health apps with their world-leading app assessment process. ORCHA’s process helps the app developer workforce by guiding their compliance toward national assessment schemes. At the same time, consumers can access the ORCHA platform to view app assessment ratings and help them make informed decisions about which apps to use or recommend.
In regards to the challenges faced by our healthcare services today including the need for more prevention, self-management and patient education, Fiona said, “As healthcare leaders and industry leaders, it’s our responsibility to drive that innovation, safely and effectively and minimise barriers.”
Prof. Daniel Fung, CEO of the Institute for Mental Health, Singapore was next to take the stage. Daniel spoke about viewing mental illness not on a spectrum, but as different dimensions: mental illness, mental health, and mental sickness and stigma.
Daniel talked through some of the digital solutions being implemented currently in Singapore. These include the Beyond the Label campaign which addresses social and self-stigma, and mindline.sg which provides a digital website and portal with a CBT-like conversational agent to help navigate Singaporeans toward help.
He concluded by emphasising the need for a further evidence base, and for partnerships within healthcare and beyond i.e. into the industry, the community, and social and educational institutions.
Future Workforce Development
The Future Workforce Development “Brag and Steal” session was opened by Dr. Judy Kuriansky. Dr. Judy teaches a course about Mental Health and the United Nations (UN) at Columbia University Teachers College in the United States.
Judy spoke about her approach to training future practitioners in a new paradigm; going beyond the traditional scientist-practitioner model and adding in a third dimension which is advocacy. Judy’s course is about developing the future workforce to not just be researchers or clinicians, but also advocates at a diplomatic level for the patients and communities they serve.
Digital tech has transformed the teaching of her course throughout the pandemic, and Judy described how a hybrid model has eventuated as the sweet spot which parallels the inclusion of digital tools in the mental health ecosystem.
She acknowledged there are pros and cons to both in-person and digital, but said that while digital isn’t here to replace traditional face to face methods, it can be a powerful enabler, a way to increase access, and a way to provide service users with choice.
Dr. Tania Wilson is a Clinical Psychologist and General Manager of ProCare, one of the largest primary health organisations in New Zealand.
Tania’s angle on workforce development was sharing the lessons she and her organisation learnt when upskilling primary care workers to integrate digital mental health into their practice during the Covid-19 Pandemic.
80% of the ProCare team now report that digital tools are a valuable part of their practice, and the use of tools has increased from nearly 0% before the training, to about 30% today.
Key lessons from this experience were:
- Start with your leadership team. If the leaders aren’t onboard, the clinicians won’t be, so digital approaches need to be championed from the top down.
- The importance of thorough training. Clinicians need to develop confidence in the tools to bring digital to life in their practice. It’s about more than just making them aware of it, it’s spending time to ensure they understand and are confident in using and prescribing the tools.
Ashley de Silva, CEO of ReachOut in Australia, spoke about their recently launched PeerChat service, and how launching the 1:1 Peer Chat Service went beyond introducing a new service to developing a whole new workforce.
The activation of Peer Support Workers required shifting the culture at ReachOut, not only within the Peer Support Workers themselves, but also the non-Peer Support Workers in the rest of the organisation.
Peer workers had described their experience in the workforce as being at the bottom of the hierarchy in clinics and other settings. “They felt that their experience was not appreciated or understood, and for ReachOut this was relevant to really building an organisational culture to support them.”
To build a supportive culture, ReachOut made sure that the Senior Manager of the Peer Team is a peer support worker, not a clinician. Ashley explained that this was crucial to shifting the perspective of Peer Support Workers as being an adjunct or an alternative, towards being seen as the professionals that they are.
Brag & Steal: eMental Health Innovation
Rachel Green is the CEO of SANE Australia, and is a fierce leader with her own lived experience. She joined SANE in mid-2021 with the ultimate goal of ending mental health inequity through systemic change. She said, “We use more tech analytics and data in online shoe shopping than in mental health and suicide prevention” which highlights the untapped potential technology has to improve mental health care.
A key concept Rachel spoke to, is the notion that patient record systems historically replicate old power dynamics – they are built as a back-of-house system by providers to meet provider needs, rather than serving the patient or service user.
In response, SANE has built a service that offers guided support to people through the mental health system via an app that was co-designed with 60 co-designers. Users are welcomed, on boarded, befriended, and offered counselling and peer support through the portal.
Within SANE, lived experience leads at every level, which Rachel said is a must-have within the mental health industry. “By encouraging people towards our online forums, that then becomes the platform from which we recruit into leadership programmes and learn what people think to shape our advocacy.”
Prof. Andy Greenshaw is a researcher at the University of Alberta. His talk discussed the immense potential of AI to solve many ‘wicked’ problems in our mental health systems, and what is currently stopping us from realising that potential.
He described AI as “an entity that will do something in a way that people can’t, but people are necessary to understand what’s needed and what should be done.”
One good idea for ‘what’, is tackling the inefficiencies we face in our systems of care. Andy described how AI has the potential to compute data in a way that human beings never could, and this data could be used to help drive innovation, systems development and solutions to some of our biggest challenges. For example, if allowed, AI could be used to calculate determinants of health such as risk of suicide to a degree far more precise than any human can, during a consult.
Another idea is considering the way we think about privacy and confidentiality when it comes to big data. While acknowledging that there are risks of misuse of data, by restricting it we are also preventing the use of this data for immense good and progress.
Dr. Laura Franch has worked in AI and robotics labs all around the world. She acknowledged that “It is easy to criticise the potentially harmful uses that technology robots and AI can have on human behaviour. What is more challenging is to find ways to effectively use these technologies for positive behavioural change.”
In an inspiring presentation, Laura highlighted three examples of AI and robots being used in innovative and positive ways:
- Digital avatars – creating a virtual copy of yourself has shown considerable promise in reducing social phobia and public speaking anxiety. By practising engaging with others from within a safe, virtual environment, participants in a study were able to address their distorted self-image caused by previous negative experiences and increase their self-confidence.
- Social robots – ‘robot therapists’ were used in one study to help students improve their wellbeing by applying principles of Positive Psychology.
- Conversational agents – robots programmed as ‘life coaches’ helped study participants improve their personal growth initiative, life satisfaction and emotional wellbeing.
Anna Elders’ theme was Connection and Whakawhānaungatanga: the Process of Establishing and Nurturing Relationships.
Anna has championed the development and implementation of Just A Thought, an eCBT tool, across New Zealand and spoke to the importance of connecting and collaborating throughout Just A Thought’s journey so far, and for the future expansion of the tool.
Anna discussed how collaboration enabled Just A Thought to emerge from Australian sister company This Way Up, and how by not reinventing the wheel an eCBT tool was able to be implemented and scaled in New Zealand at a much faster rate.
Anna described relationships and collaboration as the quickest route to success; by sharing our knowledge and tools with others we can help digital mental health grow rapidly around the world, in the same way Just A Thought has and is continuing to grow in New Zealand.
Lunch Break

Congress participants were free to enjoy a catered lunch before heading back for the afternoon sessions.
Special Interest Group: International Phone and Text Helplines
After lunch we commenced the International Phone and Text Helpline symposium, hosted by Andrew Slater, CEO of Whakarongorau (New Zealand’s national telehealth service).
The panel included Victoria Hornby OBE from Mental Health Innovations in the UK, James Wright from 988 in the US, and Dena Trujilli CEO of Crisis Text Line in the US.
Andrew opened the session by describing the purpose of Whakarongorau as “Giving everyone the opportunity for wellness, using the connected world of digital care and bringing imagination to that.”
Andrew played a powerful video which illustrated beautifully the work and the impact that Whakarongorau has, and described the immense growth and transformation that has occurred within telehealth since the pandemic, saying, “We used to be the safety net, now we’re the backbone.”
Victoria walked us through the development of SHOUT – the national mental health text line in the UK which was primarily developed through the pandemic in collaboration with Crisis Text Line in the US and other existing services.
She said that before SHOUT, “people were being encouraged to talk about their mental health, but there weren’t enough places for people to talk about their mental health. Young people were increasingly looking online for help and support.”
Of the users of SHOUT
- 40% of people who contact us have never spoken to someone about how they’re feeling,
- 55% don’t feel they have anyone to talk to.
- The vast majority of people who contact us don’t think they are worthy of help and support.
“Signposting them on to where they can get help, we think, is absolutely crucial”, Victoria said.
James Wright, CEO of 988 in the US was next to join the panel.
In a once in a lifetime opportunity to reimagine crisis services, James described how the Suicide & Crisis Lifeline was moved to a national 988 dialing code — a toll-free, easy to access helpline available to to anyone in suicidal crisis or emotional distress.
The implementation of the service has been received with demand. Comparing the same month year to year, there was a 195% increase in chat usage, and a 1,074% increase in text services. The majority of users are aged under 25, and 80% of those individuals reported being suicidal at the time of contact or in the recent past. This signals a strong opportunity to shape a generation that reaches out and utilizes 988 services for support.
Dena Trujillo, CEO of Crisis Text Line in the US was the final speaker of this session.
The purpose of Crisis Text Line is to build an empathetic world where no one feels alone. Of their service users, Dena explained that 65% of people who text into CTL share something new that they have never shared with anyone else, and 28% of people who text in, do not have any kind of support – including talking to family and friends.
Dena described CTL as a mental health emergency room — the full spectrum from triaging suicide risk right down to anxiety and relationship issues. The staffing model CTL used is having few clinicians (there are 200 staff and 55,000 volunteers). Anecdotally, CTL knows that their users see so much value in the support they receive, that a significant number go on to become volunteers.
Special Interest Group: Ethics and Law in eMental Health
eMHIC’s Special Interest Group on Law and Ethics in eMental Health is Co-Chaired by Dr Piers Gooding, Senior Research Fellow at the University of Melbourne Law School in Australia, and Richman Wee, Academic Research Manager at Te Piringa – Faculty of Law at Waikato University in New Zealand.
Piers and Richman joined the Congress to provide an update on the Position Statement that the group produced in 2021. While the Position Statement was well received globally, the Special Interest Group is expanding and aiming to take the conversations further, around emerging legal and ethical questions — to advance the thinking and indeed the doing.
Ikenna Ebuenyi, Assistant Professor at University of Pittsburgh and Smriti Joshi, Chief Psychologist at Wysa – new members of the Special Interest Group – then shared the fresh perspective they are bringing to the development of the document.
Ikenna spoke to the importance of developing the Position Statement to be relevant and inclusive of low income and resource settings. Smriti spoke about ensuring that the Position Statement is not only something that guides higher level strategy and policy, but also guides organisation, service providers, start ups, clinicians, and service users i.e. all stakeholders, and bridges the gaps from translating existing guidelines into actionable steps.

Richman Wee, Senior Researcher, University of Waikato, New Zealand and Piers Gooding, Senior Research Fellow, University of Melbourne, Australia
eMental Health Implementation Leadership Awards
The awards ceremony commenced at 3:00 PM, chaired by eMHIC Board Chair Christine Morgan. Christine recognised the importance of the eMHIC awards saying, “this one of the most important parts of the day when we can stop and celebrate wonderful achievements in this area in which we are all so passionate.”
The Leadership Awards were presented to recipients by eMHIC Board Members and key Country representatives. Winners each took the stage to receive their award and say a few words.
Congratulations to this year’s award recipients for your remarkable achievements and contributions to the development and implementation of eMental Health solutions at scale.
Award winner details can be found in the eMental Health Hall of Fame.
Following a few brief closing remarks from Anil Thapliyal and Christine Morgan, Kaumatua George Hill returned to the stage to offer a closing prayer. This was followed by a group waiata (Māori song) which concluded Day 1 of the Congress.
Participants attending in-person at the Pullman Hotel then made their way to the foyer for drinks and nibbles, to share feedback on the day and discuss exciting possibilities for future collaboration.
Friday 11th November
MC Taimi Allan extended a warm welcome back to Congress attendees around the world watching the Day 2 “Virtual Congress”, live streamed on eMHIC’s interactive online platform. She thanked the team in the virtual studio along with eMHIC’s Congress sponsors for their generous contributions, before welcoming Christine Morgan to commence the second half of the eMental Health Implementation Awards.
Congratulations to our Award Winners for your achievements in implementing digital mental health solutions at scale. You are each making an impressive and influential difference.
All award winner details can be found in the eMental Health Hall of Fame.
Keynote: Victoria Hornby OBE
Victoria Hornby, CEO of Mental Health Innovations in the UK presented on the work of SHOUT – the UK’s only 24/7 crisis text messaging mental health support service.
Key takeaway messages:
- Spikes in SHOUT’s crisis text service use tend to align with events in the media. These have included a high profile case of suicide and various TikTok posts going viral.
- 79% of users are female, 35% identify as LGBTQ+and 65% of texters are under the age of 65.
- SHOUT is reaching underserved groups, with 26% of school-aged users eligible for free school meals and relatively high representation from the Autistic and Deaf communities.
- The most common topic service users want to talk about is suicide (34%), followed by depression/ sadness (33%), Anxiety/ stress (32%), relationships (27%), Isolation/ loneliness (18%) and self-harm (15%).
- Issues experienced by people change over time. For example, suicidal ideation peaks in the 18-24 age group, while self-harm is highest for ages 13 and under.
SHOUT has partnered with the Imperial College of London to do research using parts of SHOUT’s 1.5 million conversation dataset. The aim of this is to improve training of their volunteers, as well as to advance knowledge.
In addition, SHOUT is making use of Natural Language Processing and AI to generate insights on current and emerging needs so they can build new tools to help those in need at scale.
Government Lead Initiatives Around the World
Fraser Ratchford, Vice President of Strategic Relations at Stepped Care Solutions delivered a presentation on Wellness Together Canada (WTC), a federal government funded initiative.
WTC is a free, 24/7, 1-stop virtual service for all people in Canada with over 500 resources to support wellbeing. Resources include wellness information, one-on-one sessions with a counsellor, and communities of support; all accessible via the companion app, “Pocketwell”.
WTC is underpinned by SteppedCare 2.0, a service delivery framework with different levels of intensity across the wellbeing continuum that users can self-select and move between. WTC was also formed through a process of engagement and co-design, without which the service would not be as robust or effective for those who use it.
Highlights of the service include the option to be connected with a programme navigation person, and a minimal wait-time to be connected to a counsellor (currently the longest wait-time is only 3 minutes).
Fraser said that when asked how we can achieve an equitable mental health system, it comes down to one thing — reducing any and all barriers.
“It’s not just one size fits all. People can choose between all the services to find the resource that they feel is most appropriate to them.”
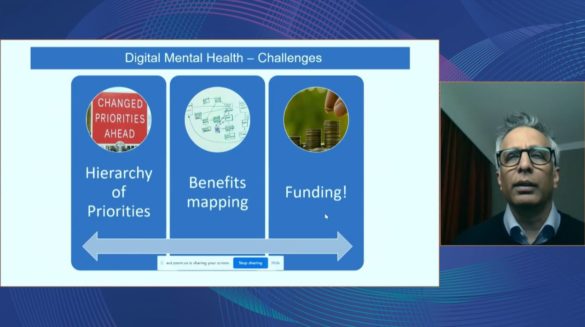
Shaaz Mahboob, Head of Digital Development, London Region, NHS, joined us to share the challenges faced by the NHS when implementing system-wide eMental Health programmes.
One major challenge, is a difficulty mapping the benefits of implementing eMental Health programmes. This includes demonstrating in a tangible way the overall success of eMental Health programmes and understanding the impact of improved mental health outcomes on the wider economy.
Another challenge is securing the necessary funding to implement eMental Health programmes at scale. If there is no cash releasing benefit, then return on investment is almost impossible to measure.
Last but not least, who pays for it? According to Shaaz, a question many ask is “Should it be a mental health investment, or should it be paid for collectively by all of the other sectors?”
Shaaz ended his thought-provoking presentation by advising us that we will need to collaborate to overcome these key challenges if we are to embed digital mental health within mainstream systems of care.
Reaching Remote Populations
Anna Dorsey, CEO of Headlight Trust, New Zealand spoke about the work her team have been doing in Queenstown since the start of the Covid-19 pandemic to grow and build an innovative community-based model for mental health.
With no contract for service, and no allocated funding, Anna and her team have found a way to bring valuable mental health education to diverse and hard-to-reach communities. They have achieved this through a combination of in-person and digital delivery modes.
This approach has real potential to support other communities nationally and globally. It is a wonderful case study showing how a small but dedicated group of people can sow the seeds for change at local level, in a way that is scalable and sustainable. In doing so, they were able to meet the needs of diverse communities living in remote locations.
Sandy Little, Territorial Manager of the Mental Health and Community Wellness Northwest Territories (NWT) in Canada, discussed how she and her team have been navigating culture, geography and eMental Health as they implement Stepped Care 2.0 in the NWT of Canada.
Sandy pointed out a key difference in the NWT Stepped Care 2.0 model, being that it forms a circular pathway — illustrating a service user’s multiple points of access to mental health care. These include; digital mental health programmes like Strongest Families Institute, NWT helpline, KidsHelpPhone, crisis lines and Wellness Together Canada.
She described a few challenges to working with a small, geographically dispersed population spread across 33 communities, half of whom are indigenous. After acknowledging the ongoing impacts of colonisation and systemic racism, Sandy stressed the importance of shifting the power differential. This can be done by listening to communities, and giving equal weighting to non-Western (aka non-racist) forms of support. Examples of these are peer support, self-help options, and cultural activities.
She made it clear that we have ongoing work to do, saying, “Trust in our system and our care providers needs to be built, and needs to be earned every day.”
Elizabeth Broadbent, Director of AI Psychology Research at Soul Machines impressed us with an introduction to Digital People from Soul Machines; covering how they work, and what their role in mental healthcare may be in the future.
The underlying technology as Liz described it, is fascinating. Soul Machines’ Digital People have a digital brain that enables receiving and responding to stimuli, pattern recognition, machine learning, context awareness and sentiment analysis. They also have modules facilitating emotions, attention and memory.
Digital People can be programmed with role-specific skills, enabling them to become experts in any specific area. This functionality is combined with a hyper-realistic appearance and autonomous animation. As such, they are able to understand what a person is saying and form an empathetic connection with them before providing sound advice and support.
Liz explained that Digital People have already been trialed in mental healthcare. They are currently at work helping real people with stress management and loneliness. A digital worker called Florence is also in use at the World Health Organization, providing people with smoking cessation information and support in six languages.
Dr. Elizabeth Broadbent, Director of AI Psychology Research, Soul Machines
Keynote: Professor Roger McIntyre
Roger is Professor of Psychiatry and Pharmacology at the University of Toronto, is CEO of Braxia Health and has been named one of the world’s most influential scientific minds. Not surprisingly, Congress attendees were captivated by his keynote “Technology and Psychiatry Closing the Gap During the COVID-19 Pandemic in the United States”.
Roger began by explaining how Braxia was created to make psychopharmacologic therapeutics accessible to people who are resistant to traditional treatments for depression. He said that for serious mental illness, accessible treatment is crucial. This is because research shows that unlike every other area in medicine, morbidity and mortality in Psychiatry is continuing to rise, while supply of care is continuing to diminish.
To address this imbalance, Roger’s company Braxia has partnered with KetaMD, provider of an FDA-approved Ketamine treatment to make rapid-acting Ketamine treatments available to people in their homes. Braxia currently has 6 clinics in Canada. It has recently launched in Florida with plans to expand across 38 states in the United States, and has just opened a clinic in Eastern Europe.
Roger described how the KetaMD app provides a “concierge-like end-to-end client experience” where clients can easily arrange their own referrals and consultations from their mobile phone. Treatment is accompanied by a nurse-guided telehealth session with ongoing support provided through Braxia’s technology platform. Roger likened this to the “Amazon model” of delivery-of-care.
He summed up his keynote by saying that, although we hear so much about the opportunity of technology in healthcare, “There’s a huge gap when it comes to implementation science.”
“Here we have the first organisation in the United States that has really taken this best practice approach to really bring implementation science to the table.”
Brag & Steal: Supporting Parents and Families
Patricia Lingley-Pottie, Co-founder, CEO and President of the Strongest Families Institute joined us from Canada to speak to us about the work of her organisation, Strongest Families Institute (SFI).
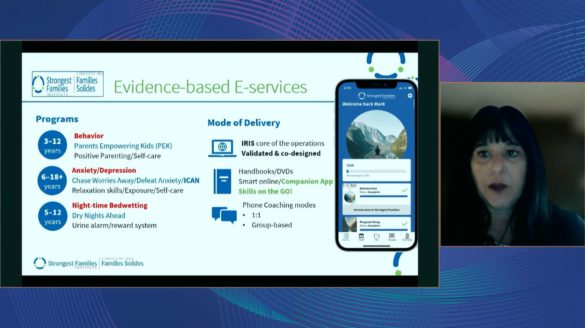
Drawing from 20+ years of social science research, SFI is helping 13k Canadians annually by delivering CBT-informed, skills and strength-based telephone coaching to families in the comfort of their home.
Trish explained how various delivery modes are now available — from telephone coaching, to the IRIS online platform, to hard-copy handbooks or DVDs, to their new companion app, “Skills on the Go”.
Co-design has been a core tenet of SFI since its inception, which helps explain why SFI has such strong outcomes and an outstanding 99% overall client satisfaction rating. When it comes to supporting neurodiverse children, Trish presented two inspiring case studies showing how neurodiverse children can benefit from co-designed, evidence-based services; as demonstrated by data showing impressive post-treatment results.
She ended her presentation by announcing that SFI is now working in partnership with the Newfoundland & Labrador Government (with funding from the Public Health Agency of Canada), to provide a stepped-care population approach. Their goal is simple: for more people to have access to their programme to prevent downstream impacts from even occurring in the first place.
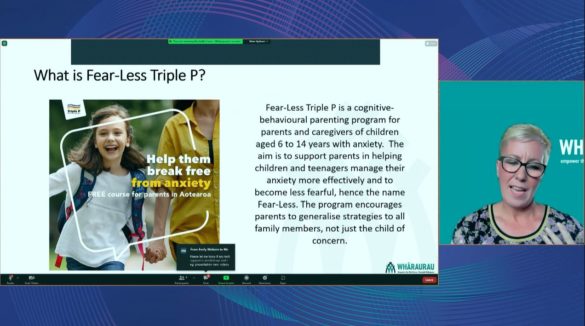
Rochelle Cave, Project Manager, Parent & Teacher Team at Whāraurau, New Zealand, introduced us to Fearless Triple P, a free cognitive behavioural parenting programme focussed on reducing anxiety and fear in children aged 6 to 14 years. Fear-less has been successful in helping thousands of parents across New Zealand learn ways to support their children to understand anxiety, develop emotional resilience and overcome avoidance — in other words, fear less.
Over Covid-19, an e-platform was found to be the most effective way to deliver their clinically-proven programme to parents and caregivers. To this day, digital modes of delivery allow Whāraurau to provide accessible and flexible support to families across New Zealand with modules that they can access and re-visit in their own time and at their own pace.
Dr. Victor (Soji) Ladele, Global Innovation Lead of Mental Health & Psychosocial Wellbeing at UNICEF shared with us UNICEF’s innovative mental health and psychosocial work portfolio.
Victor began by telling us about how current issues such as climate change, rapid urbanisation and youth unemployment are profoundly affecting the mental health of young people in ways we are yet to fully understand. As a result, we are now experiencing a period of “exponential seismic global change”, with the future of mental health looking markedly different from the past.
He explained that new opportunities to address this need are emerging, but since local development issues are complex and there is no solution that fits all circumstances, we need to act with care. As he put it, “If you board the wrong train, it is no use running along the corridor in the other direction.”
To address key challenges, the office of innovation at UNICEF is building a collective movement of human-centred design, leveraging innovative minds from 190 countries to deliver radically innovative solutions for children. These include; telehealth and community-based mental health training, using data from social media to spot trends and prevent self-harm, self-guided video games to reduce stigma, automated chatbots, USupportMe (the Uber of mental health), and leveraging data from smartphones and wearables to create more representative pools of data.
Dr. Victor (Soji) Ladele, Global Innovation Lead, Mental Health & Psychosocial Wellbeing, UNICEF
Victor warned that the interaction of technical and social systems can create unexpected outcomes. This is why at UNICEF, design as a discipline is central to the way they work.
Putting design into practice, UNICEF works from a platform in the global North, bringing in stakeholders (including young people) from the global South into the process as early as possible. This helps UNICEF to create what Victor called “a virtuous cycle of innovation.”
Brag and Steal: Product Innovation
Liz Berryman, Founder and Director of Chnnl, New Zealand joined virtually from Sydney in Australia to talk about her organization, Chnnl.
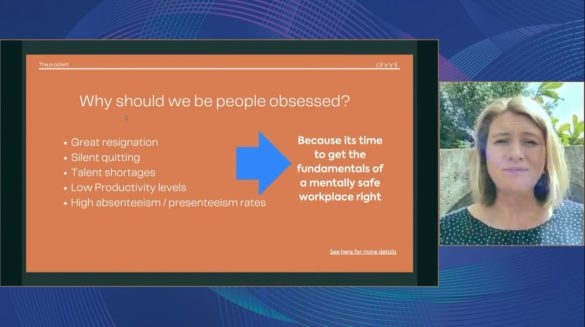
She described how the focus these days is often on good health, but Chnnl’s focus is on what good looks like in the workplace. In fact, some research says as much as 88% of our mental health can be attributed to workplace conditions, making it the perfect place to provide mental health prevention and support.
Liz talked about how Chnnl partners with around 30 organisations world-wide to help support their people through preventative data-driven measurement and reporting, real-time feedback to senior management, and connecting people early with EAP services and mental health practitioners.
Liz said, now more than ever, as we navigate the so-called Great Resignation our workplaces should all be “people obsessed”. This ensures we get the fundamentals of mental health right to realize our people’s full potential.
Umar Nizamani, Managing Director of Netherlands-based NiceDay International, shared enlightening intel on how to build Artificial Intelligence responsibly for mental healthcare.
He introduced NiceDay as a digital workspace powered by AI for therapists to use together with their clients. In an innovative departure from traditional therapy, NiceDay proposes that instead of 1-hour sessions with their therapist, clients should have 30-40 minute sessions. These shorter sessions should be combined with asynchronous time spent on the NiceDay app, to equip them with the tools and skills they need to manage their own mental health.
Bringing NiceDay’s AI technology to end-users requires them having a strong foundation of privacy-by-design architecture, including ISO standard certification and explicit research consent. In addition, NiceDay uses domain expert insights to better understand which features characterize effective therapy. It cleverly correlates these with the underlying data to generate “explainable AI for needs based care”.
By combining these elements, NiceDay is able to offer a highly effective, trusted treatment solution. One that equips clients to manage their own mental health; before, during, and after therapy sessions.
Anti-Racism, Anti-Oppression (ARAO)
Topaza Yu is a Counselling Psychology Doctoral Student at the University of North Dakota, a Member of the Prime Minister’s Youth Council, and a Board Member of Action Canada. Her focus is on the importance of discussing and practising anti-racism and anti-oppression (ARAO) in the context of eMental Health.
She presented 3 powerful examples of how we can integrate an ARAO lens in eMental Health, while urging us to view the inevitable discomfort it entails as a sign of growth.
Despite best efforts, she said “Complete safety is not guaranteed. The best we can do is create and foster safer spaces… where learning and unlearning is very much encouraged and welcomed.”
This includes being aware of unconscious biases in relation to often excluded and marginalised communities, challenging and countering racism as it arises and applying an ARAO lens at all levels of eMental Health strategy, design and implementation.
Topaza wrapped up her presentation, and the Congress in the most fitting way by reminding us of the crucial principle “There is nothing for us without us”. To achieve this, she urged us to hold onto the importance of co-designing accessible and equitable health systems and digital solutions in close collaboration with the people they were created to serve.
MC Taimi Allan summed up the Congress as doing exactly what it set out to do.
The Congress was a whirlwind of connection between governments, international experts and peers, and collaboration via an “all in” Congress group activity and eMHIC’s online networking platform. Inspiration came in the form of current best practise and exciting new initiatives demonstrated by the world’s best and brightest. Participants from around the world were left energized and full of ideas for how to make a difference in the lives of the people they serve.
Taimi finished by saying that although we are leaving the eMHIC Congress with renewed energy we must not lose sight of what is important – and that is people. To bring this home, she quoted our first Congress Keynote speaker Patricia Deegan whose message resonated with us all:
It's not about what's the matter with people but what matters to people.
Pat Deegan PhD
For further information about any of the 2022 Congress sessions, email congress@emhicglobal.com. Or to view and register for upcoming events, visit the eMHIC Events Page.